Oceanside (760) 630-9200

Neuropathy and Its Impact on Foot Health
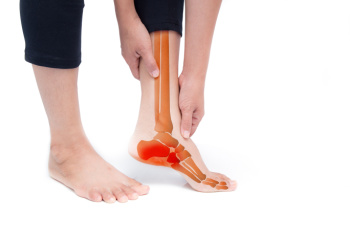
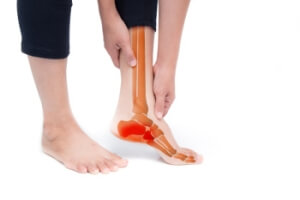
Neuropathy refers to a condition characterized by damage to the nerves, disrupting the normal communication between the brain and other parts of the body. When neuropathy affects the feet, it can lead to a range of symptoms and complications that significantly affect foot health. Neuropathy often manifests as numbness, tingling, burning sensations, or sharp pain in the feet. These symptoms can make it difficult for individuals to sense pain or temperature changes, increasing the risk of injuries and infections. Additionally, neuropathy can cause changes in foot structure and function, leading to conditions such as hammertoes, bunions, and Charcot foot. Additionally, poor blood circulation associated with neuropathy can impair wound healing, increasing the risk of ulcers and complications. It is imperative for individuals with neuropathy to prioritize foot care and regularly inspect their feet for any signs of injury or infection. Seeking timely medical attention from a podiatrist and implementing preventive measures can help manage neuropathy and preserve foot health in the long term. If you have symptoms of neuropathy in your feet, it is strongly suggested that you are under the care of a podiatrist who can help you with effective management tips.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with Dr. Jeff Brooks from Oceanside Foot & Ankle Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact our office located in Oceanside, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Neuropathy
Neuropathy is the weakness, numbness, and pain in the hands and feet due to damage to the peripheral nerves. The peripheral nerves are responsible for sending information from the brain and spinal cord to the rest of your body. Causes of Neuropathy include: traumatic injuries, infections, metabolic problems, exposure to toxins, and diabetes.
Diabetes is the most common cause, with more than half of the diabetic population developing some type of neuropathy. There are several types of neuropathy and they vary based on the damage of the nerves. Mononeuropathy is classified as only one nerve being damaged. When multiple nerves are affected, it is referred as polyneuropathy. One of the types of polyneuropathy is distal symmetric polyneuropathy. It is the most common for people with diabetes and starts when the nerves furthest away from the central nervous begin to malfunction. The symptoms begin with pain and numbness in the feet and then they travel up to the legs. A rarer form of polyneuropathy is acute symmetrical peripheral neuropathy, which is a severe type that affects nerves throughout the body and is highly associated with Guillain-Barre syndrome, an autoimmune disorder that attacks the peripheral nervous system and can be fatal. Although there are many types of neuropathy, most of them share the same symptoms such as pain, extreme sensitivity to touch, lack of coordination, muscle weakness, dizziness, and digestive problems. Since neuropathy affects the nerves, those affected should be careful of burns, infection and falling, as depleted sensations disguise such ailments.
The best way to prevent neuropathy is to manage any medical conditions such as diabetes, alcoholism, or rheumatoid arthritis. Creating and managing a healthy lifestyle can also go a long way. Having a healthy diet full of fruits, vegetables, whole grains and lean protein can keep the nerves healthy. These types of food have the nutrients to prevent neuropathy. Regularly exercising can help as well, but it is best to consult with a doctor about the right amount. In addition to diet and exercise, avoiding risk factors will also prevent neuropathy. This includes repetitive motions, cramped positions, exposure to toxic chemicals, smoking and overindulging on alcohol.
Wounds That Don't Heal Need to Be Checked
The Impact of High Heels on Walking

Wearing high heels can transform the way we walk, influencing posture and gait dynamics in subtle yet significant ways. The elevated heel of high-heeled shoes prompts a redistribution of body weight, causing the pelvis to tilt slightly forward and the spine to arch gently. This adjustment creates the illusion of longer legs and a more defined silhouette, enhancing confidence and poise. Additionally, high heels encourage shorter, more deliberate strides, leading to a smoother and more controlled walking motion. The lifted heel also engages the calf muscles and accentuates the curve of the buttocks, contributing to a more graceful and elegant stride. Despite these perceived benefits, it is important to note that prolonged wear of high heels can place strain on the feet, ankles, and lower back, potentially leading to discomfort and musculoskeletal issues over time. So, while high heels can indeed enhance the aesthetic appeal of walking, it is essential to strike a balance between style and comfort for optimal foot health. If you would like more information about the effect high heels have on walking, it is suggested that you consult a podiatrist.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact Dr. Jeff Brooks from Oceanside Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
- Ankle Joints
- Achilles Tendon – May shorten and stiffen with prolonged wear
- Balls of the Feet
- Knees – Heels cause the knees to bend constantly, creating stress on them
- Back – They decrease the spine’s ability to absorb shock, which may lead to back pain. The vertebrae of the lower back may compress.
What Kinds of Foot Problems Can Develop from Wearing High Heels?
- Corns
- Calluses
- Hammertoe
- Bunions
- Morton’s Neuroma
- Plantar Fasciitis
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact our office located in Oceanside, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Why High Heels Are Not Ideal for Healthy Feet
It is no secret that high heels are uncomfortable to wear for long periods of time. Although beauty is pain, you should not sacrifice the health of your feet for a stylish heel. Wearing high heels can potentially cause many different foot conditions that may be avoided by wearing proper footwear.
The structure of high heels forces weight of your body to get shifted forward toward the ball of the foot. The higher the heel you wear, the more weight and pressure get shifted forward. The pressure that your toes may experience from wearing heels may lead to hammer toes, bunions, and ingrown toenails. Extra weight and pressure resulting from wearing heels may cause stress fractures. Furthermore, heels may cause pinched nerves which may result in Morton’s neuroma.
High heels are even more dangerous for people who are clumsy. Falling or tripping while wearing heels can cause an ankle sprain or twist.
What many people don’t know is that heels can also cause back and knee problems. In order for your body to stay balanced on heels, your spine has to sway unnaturally, which adds stress to your spine muscles. This may cause you to experience a sore lower back.
If you decide to wear high heels regardless of the risks associated with them, there are ways you can minimize their harmful effects. One way to reduce injury is to massage and stretch your legs at the end of the day. Stretching can prevent the Achilles tendons and calf muscles from becoming too tight. If you are simply looking for more height, wedges and platforms provide a better surface area to distribute the body weight across compared to thinner heels.
If you experience pain from wearing high heels, it is important to see a podiatrist before any of your symptoms become worse.
Athletic Advantages for Flat-Footed Children

Flat feet, which are often considered to be a hindrance to athletes, need not deter children aged 11 to 15 years from pursuing their athletic aspirations. Flat feet may lack the arch typically associated with athletic prowess, but they can offer unique advantages in various sports. For instance, individuals with flat feet tend to have increased stability and a lower center of gravity, which can enhance balance and agility in activities such as gymnastics, martial arts, and dance. Additionally, the absence of a pronounced arch allows for greater surface contact with the ground, facilitating better shock absorption and energy transfer during running and jumping. With proper training, footwear selection, and the use of orthotics, children with flat feet can excel in sports and lead active lifestyles without limitations. If your child has flat feet, and is interested in participating in sporting activities, it is suggested that you consult a podiatrist who can accurately address any concerns you may have.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Dr. Jeff Brooks from Oceanside Foot & Ankle Center. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our office located in Oceanside, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What is Flexible Flat Foot?
Flatfoot is classified as having the entire sole of the foot in contact or near contact to the ground while standing. The disorder is also known as fallen arches, because those affected have no arch in their feet. Flexible flatfoot and rigid flatfoot are the two types of flatfoot.
A person has flexible flatfoot if when sitting or standing on their toes, they have an arch that disappears when they stand with the entire foot on the ground. Flexible flatfoot may also be called “pediatric flatfoot” because the condition first appears in childhood. It is common among infants because the arch does not develop until the age of 5 or 6 years. Rigid flatfoot is not as common in children as it is with adults. This type of flatfoot is developed due to the weakening of tibialis posterior muscle tendon, a major supporting structure of the foot arch. Development of this deformity is progressive and shows early signs of pain and swelling that begins at the inside arch of the foot and moves to the outside of the foot below the ankle. More severe cases can possibly lead to arthritis of the foot and ankle joints.
Although most cases of flatfoot involve people born with the condition, some less common causes are obesity, diabetes, pregnancy, and osteoporosis. In some cases, flatfoot may come with no symptoms at all and does not require any type of treatment. With other cases though, symptoms may include pain in the shin, knee, hips and lower back. If a person with flatfeet experiences such symptoms, a health care provider may suggest using orthotic devices or arch supports, which may reduce the pain. Wearing supportive shoes can also prove more comfortable with flatfeet and staying away from shoes with little support such as sandals. Other methods to relieve pain also include stretching the Achilles tendon properly and using proper form when doing any physical activity. In addition, losing weight can reduce the stress on your feet and reduce the pain.
Causes and Characteristics of Plantar Warts
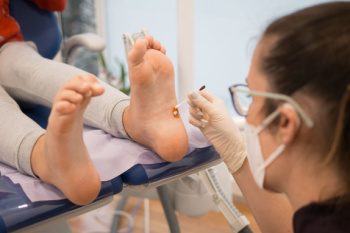
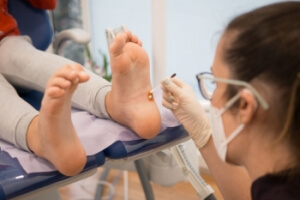
Plantar warts, though benign, are contagious and can be a source of discomfort for many individuals. These small, grainy growths typically develop on the soles of the feet, particularly in areas that bear weight such as the heel or ball of the feet. Plantar warts are caused by the human papillomavirus, or HPV, specifically strains that thrive in warm, moist environments. Plantar warts often enter the body through tiny cuts or breaks in the skin. Walking barefoot in public places like locker rooms, swimming pools, or communal showers can increase the risk of exposure to the virus. Additionally, individuals with weakened immune systems or compromised skin integrity are more susceptible to developing plantar warts. The pressure and friction exerted on the feet during walking can flatten plantar warts, causing them to grow inward and become painful. While plantar warts may resolve on their own over time, seeking treatment from a podiatrist can help alleviate discomfort and prevent them from spreading to other areas of the feet or to other individuals. If you have developed a plantar wart, it is suggested that you visit a podiatrist who can offer effective treatment solutions.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Jeff Brooks from Oceanside Foot & Ankle Center. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in Oceanside, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.